Historic Medicaid Cuts Are Reshaping Health Care in Arizona
Medicaid and the Arizona Health Care Cost Containment System (AHCCCS) are crucial to keeping Arizonans healthy. But recent federal cuts to Medicaid will ripple through the state’s health system and pose risks for patients and providers, especially rural hospitals. Here’s what these Medicaid cuts mean for Arizona:
A Nearly $1 Trillion Cut to Medicaid
Medicaid is a program funded jointly by states and the federal government that provides health coverage to low-income families and individuals. So when funding evaporates, patients suffer. In July 2025, Congress enacted the Republican Tax Law (H.R. 1), which included the largest Medicaid cuts in history – $930 billion over the next decade – in order to fund tax breaks that are skewed toward the wealthy and big corporations.
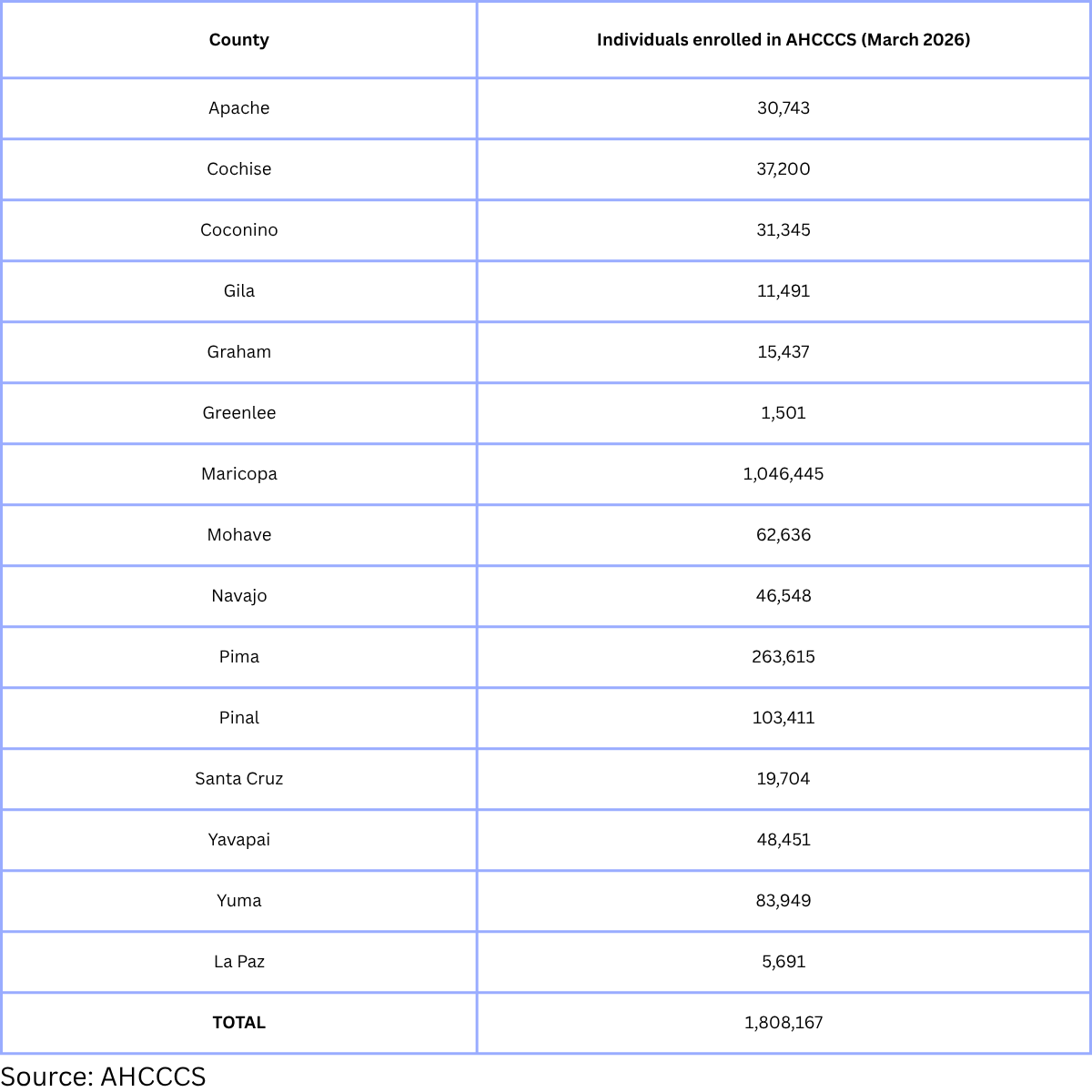
These cuts could have startling implications for the 1.8 million Arizonans who receive coverage through AHCCCS, the state’s Medicaid program, in every county across the state:
Arizona Hospitals Face Service Cuts and Closures
These funding cuts could lead to staffing reductions, service cuts, and hospital closures as hospitals lose revenue from AHCCCS reimbursements tied to Medicaid coverage. Medicaid reimbursements help cover the cost of care, so when that funding declines, hospitals must make up the difference by cutting services or staff. More than 300 hospitals nationwide are at risk for closure. In Arizona, seven hospitals are currently considered to be at risk of cuts, including Phoenix Children’s Hospital. Northern Arizona Health Care in Flagstaff cancelled a planned expansion due to the cuts. Another Flagstaff hospital – North Country HealthCare – struggled with other federal cuts in 2025 and eventually had to file for bankruptcy.
Rural Arizona Hit the Hardest
In addition to hospital closures, Medicaid cuts will devastate rural economies and leave patients strapped for care. Many rural hospitals are already financially unstable – 44% are already operating at a loss, and nearly 100 have closed in the last decade. Several Arizona counties already have fewer than one OB-GYN per 10,000 women, and the situation could worsen if rural hospitals close. In rural counties within commuting distance of a hospital, hospitals employ 10 percent of the workforce. More than 300 rural hospitals are at immediate risk of closure, particularly with H.R. 1’s cuts now in effect.
Five rural hospitals in Arizona, which collectively serve up to 400,000 Arizonans, are considered to be at-risk of closure. Neal Jenson is the CEO of one such hospital, Cobre Valley Regional Medical Center in Globe, a rural health care center with around a third of its patients on Medicaid. “What [the law is] going to do to rural health care in Arizona is destroying it,” said Jenson. “Anytime you jeopardize a third of your payer base, you will have a significant impact.”
Vulnerable Arizonans Face the Biggest Risks
People with disabilities and the elderly may also be adversely affected by H.R. 1’s cuts. Because of higher levels of health care spending and lower rates of employment, people with disabilities tend to rely more on Medicaid than other populations. Research shows that when federal Medicaid funding is reduced, state programs like AHCCCS typically begin by cutting optional benefits like home- and community-based services (HCBS) that these groups rely on. At the same time, the law introduces harsh red-tape requirements that could push eligible people with disabilities and the elderly off Medicaid simply because they cannot navigate the paperwork, meet the requirements, or consistently verify employment.
The Economic Fallout Could Reach Far Beyond Health Care
When funding for Medicaid is reduced, health care providers lose revenue, cut spending, and lay off workers, and then those workers spend less money in local economies. Experts estimate that H.R. 1, due to its cuts to Medicaid and the Supplemental Nutrition Assistance Program (SNAP), could increase the national unemployment rate by roughly 0.8 percentage points, equivalent to losing more than 1.2 million jobs. Arizona will be hit harder than average, with a relative 1.4% increase in unemployment. States are also facing budget strain because they must absorb losses while their tax revenues decline due to reduced economic activity and H.R. 1’s limits on provider taxes – state taxes on health care providers that states use to finance Medicaid. This decrease in state revenue could lead to tax increases, cuts to Medicaid services or eligibility, and reductions to other services like education and infrastructure. Arizona is projected to have deeper losses than most states: 21.1% of its federal Medicaid funding, compared, for example, to Wyoming’s 5.5%. If 80% of funding is reduced, Arizona has a trigger law on the books where Medicaid expansion eligibility will be terminated. This would mean the automatic elimination of affordable coverage for, as of 2025, over half a million Arizonans – with no action required by the state legislature.
The Rural Health Fund Won’t Replace the Lost Medicaid Funding
The main Congressional Republican response has been to highlight the budget reconciliation law’s $50 billion rural health fund. GOP lawmakers argue that this program represents the largest federal investment in rural health care in decades and is designed to stabilize struggling rural hospitals and providers. However, the fund cannot compensate for the size of the cuts in the legislation. Despite its name, most of the money in the law is not even targeted at rural communities. And states can use only up to 15% of their funding to pay providers for patient care. All told, it would only offset about 37% of the Medicaid funding losses expected in rural areas – and many of the biggest federal spending reductions will occur after the fund expires in 2030. Even less useful: Arizona is only slated to receive $167 million from the rural health fund, the sixth-lowest amount in the nation.
For the nearly 1.8 million Arizonans who rely on Medicaid, the consequences of these cuts may be just beginning. The impact will be felt in hospitals, rural towns, and the lives of patients who depend on care.